I have four pancakes before a game, covered in syrup or honey. I swear to God, it’s the best thing – it has changed this season.
I have four pancakes before a game, covered in syrup or honey. I swear to God, it’s the best thing – it has changed this season.
When I joined the club, I could see the players eating them and thought to myself, “What is going on here?”
But honestly, it’s been a game changer.
I don’t understand the science behind it, but it gives me such a high energy boost. I think that’s why I’m able to rattle around the pitch so much.
めぐりあう書物たちもどき
めぐりあう書物たち/尾関章
「読む」「考える」の by chance
2023年12月1日 投稿者: AKIRA OZEKI
休載のお知らせ
https://ozekibook.com/2023/12/01/休載のお知らせ/
**
毎週 楽しみにしていた 尾関章さんの「めぐりあう書物たち」が「筆者のやむを得ない事情により」しばらく休むとのこと。毎週金曜日に受けていた刺激が急になくなり、仕方なく(尾関さんにメールするという形で)自分で刺激を作り出すことにした。
以下は、そのログ。「めぐりあう書物たち」の形式をそのまま踏襲したのだが、尾関章さんほどの格調は出せていない。
**
金曜日(22)2024年5月17日(金)
今週の書物/名郷直樹『いずれくる死にそなえない』
http://www.kushima.org/?p=66690#comment-237927
金曜日(21)2024年5月10日(金)
今週の書物/京都に咲く一輪の薔薇『京都に咲く一輪の薔薇』
http://www.kushima.org/?p=70986#comment-237762
金曜日(20)2024年5月3日(金)
今週の書物/Harry Cliff『How to Make an Apple Pie from Scratch』
http://www.kushima.org/?p=75038#comment-237550
金曜日(19)2024年4月26日(金)
今週の書物/Bruno Latour『Face à Gaïa. Huit conférences sur le nouveau régime climatique』
http://www.kushima.org/?p=74991#comment-237508
金曜日(18)2024年4月19日(金)
今週の書物/近藤祐『〈狭さ〉の美学』
http://www.kushima.org/?p=66054#comment-237394
金曜日(17)2024年4月12日(金)
今週の書物/Leonard Koren『Wabi-Sabi for Artists, Designers, Poets & Philosophers』
http://www.kushima.org/?p=25282#comment-237325
金曜日(16)2024年4月5日(金)
今週の書物/広井良則『人口減少社会のデザイン』
http://www.kushima.org/?p=71768#comment-237209
金曜日(15)2024年3月29日(金)
今週の書物/尹雄大『つながり過ぎないでいい』
http://www.kushima.org/?p=68309#comment-237049
金曜日(14)2024年3月22日(金)
今週の書物/日下渉『反市民の政治学』
http://www.kushima.org/?p=71191#comment-236910
金曜日(13)2024年3月15日(金)
今週の書物/John Hersey『Hiroshima』
http://www.kushima.org/?p=76110#comment-236689
金曜日(12)2024年3月8日(金)
今週の書物/Paul Shapiro『Clean Meat』
http://www.kushima.org/?p=76085#comment-236506
金曜日(11)2024年3月1日(金)
今週の書物/ミヒャエル・エンデ『モモ』
http://www.kushima.org/?p=76044#comment-236411
金曜日(10)2024年2月23日(金)
今週の書物/河口慧海『チベット旅行記』
http://www.kushima.org/?p=75936#comment-236338
金曜日(9)2024年2月9日(金)
今週の書物/藤沢周平『日暮れ竹河岸』
http://www.kushima.org/?p=45511#comment-236059
金曜日(8)2024年2月2日(金)
今週の書物/Francis Jammes『Le Roman du Lièvre』
http://www.kushima.org/?p=75846#comment-235901
金曜日(7)2024年1月26日(金)
今週の書物/Alexis de Tocqueville『Democracy In America (Volume 2)』
http://www.kushima.org/?p=75820#comment-235737
金曜日(6)2024年1月19日(金)
今週の書物/石牟礼道子『椿の海の記』
http://www.kushima.org/?p=75796#comment-235656
金曜日(5)2024年1月12日(金)
今週の書物/Carlo Rovelli『White Holes』
http://www.kushima.org/?p=75664#comment-235498
金曜日(4)2024年1月5日(金)
今週の書物/青木玉『小石川の家』
http://www.kushima.org/?p=75596#comment-235353
金曜日(3)2023年12月29日(金)
今週の書物/坂口弘『歌集 常しへの道』
http://www.kushima.org/?p=14955#comment-235201
金曜日(2)2023年12月22日(金)
今週の書物/Fernando Pessoa『The Book of Disquiet: The Complete Edition』
http://www.kushima.org/?p=75351#comment-235037
金曜日(1)2023年12月15日(金)
今週の書物/幸田文『きもの』
http://www.kushima.org/?p=75297#comment-234917
Anti-China sentiment in America
After years of living in dorms and subpar apartments, Lisa Li could not wait to close on her new home.
The one-bedroom condo in Miami’s financial district had a view of the river, was in a safe neighborhood and, Ms. Li heard, had neighbors who were much like her — less party, more chill. So Ms. Li, a 28-year-old who came to the United States 11 years ago as a college student from China, put in an offer, had her bid accepted and began ordering furniture.
Then things took a sharp turn. At the last minute, the title company raised concerns about a small United States Coast Guard outpost near South Beach a few miles away. Her purchase, the company said, might run afoul of a new Florida law that prohibits many Chinese citizens from buying property in the state, especially near military installations, airports or refineries.
Under the law, Ms. Li could face prison time, and the sellers and real estate agents could be held liable. The deal collapsed.
More than three dozen states have enacted or are considering similar laws restricting land purchases by Chinese citizens and companies, arguing that such transactions are a growing threat to national security and that the federal government has failed to stop Chinese Communist Party influence in America.
花のこころ(山本静山)
人間の世界には、ずいぶんとむだが多いように思えますが、そのむだが、なかなかたいせつなのです。
山へ登り、野にさまよい、または旅の車中から、ただ何とはなしに、あたりの風景をながめている。そのなにげなくながめているということが、数多く重なってゆくにつれて、自然の美しさ、草や木の在り方が、心の目に写されてゆくのです。そうして花を生けるときに、いつとはなしにそのことが、大きく役立っていることに気がつきます。おもしろいことです。
At home with Leonard Koren
Richarlison
State of Southeast Asia Survey (ASEAN Studies Centre, ISEAS – Yusof Ishak Institute)
Findings from the latest State of Southeast Asia Survey conducted by the ASEAN Studies Centre at the ISEAS – Yusof Ishak Institute reveal that Southeast Asia’s top preoccupations are with recessionary pressures, intensifying economic tensions between major powers, as well as geopolitical concerns over the ongoing Israel-Hamas conflict and aggressive behaviour in the South China Sea. ASEAN’s inability to cope with fluid political and economic developments continues to worry the region.
China remains the most influential economic and political-strategic power in the region while the US has experienced a decline in its popularity in the event of a forced choice. China also tops the charts in terms of strategic relevance to ASEAN, outpacing the US by a narrow margin, while Japan remains as the most trusted major power in the region.
重信房子
ああ友よなぜ留まったのか雪山に卑怯になれない君の過ち
辻口博啓
蓬萊邨
Dar Mima
Yazid Ichemrahen
雪林の一隅(久保孝久)
爲末大 Dai Tamesue @daijapan
今回の大谷さんの話とは関係なく(いやないこともないですが)ですが、ふと思ったので。
一般的に、アスリートが有名になり始める年齢は18-24歳あたりで、そこで以下のようなことが起こります。
・先輩や昔の同級生が保険を売りにきたり、お金を貸して欲しいとお願いされる。
・いろんな人を紹介される。その中にグレーゾーンの人が混ざっていることもある。紹介する人は先輩だったりするのでややこしい。
・マネジメント事務所から連絡がある。
・会社を作る必要が出てきた場合、よくわからないまま株主の比率が決まる。
田舎で育った場合のアスリートは、昔と同じように素直に生きているといいように転がされてしまいます。
それで傷ついた人は今度は警戒心が強くなり、とにかく知っている数人だけで固めようとしますが、それはそれで身内と近くなりすぎて問題が起きたりします。
難しいのはそれが競技に集中している時であり、さらに20代の経験がない若い時にやってくる点です。相談しようにも、スポーツの中にそんな経験がある人も少ないです。言いにくいことも多い。
最近は少しマシになっていると思いますが、それでもやっぱりちらほら困っている話を聞き、なんとかできないだろうかと考えています。
Science Fictions (Stuart Ritchie)
Science, the discipline in which we should find the harshest scepticism, the most pin-sharp rationality and the hardest-headed empiricism, has become home to a dizzying array of incompetence, delusion, lies and self-deception.
税務調査官の悩み(片山会計事務所グループ)
日本国憲法30条 国民は、法律の定めるところにより、納税の義務を負う
日本国憲法84条 あらたに租税を課し、または現行の租税を変更するには、法律又は法律の定める条件によることを必要とする
この憲法84条の規定を課税要件法定主義と呼んでいます。税務調査での課税は必ずしもこの課税要件法定主義を充たしてはいません。つまり本来は課税要件の法律根拠が存在せず、憲法規定上は課税できないものを、調査官達は厳しい調査件数ノルマで無理な課税を行っているものがかなり含まれている訳で、これは課税庁側の更正決定処分で行われる課税ではなく修正申告書の提出といった形で「自主的」に申告を済ませている以上は決して表には出てきません。この事は少なからず良心的な調査官達を自己矛盾で苦しめている事となります。
国税庁は法律よりも「通達」で課税を行う事が一般的です。通達とは、国家行政組織法14条2項により大臣が下級庁に対して発するもので、問題になるのは法律の解釈を大臣または長官が決めてしまう解釈通達です。解釈通達は、例えば国税庁長官が発したものでしたら、国税庁の下級庁である国税局や税務署員は必ずこの解釈に拘束されますが、下級庁の職員以外の一般国民はその解釈に縛られる事はなく自由な租税解釈権を有しています。
通達とは国民に選ばれた国会議員により国会で審議されて可決された法律ではなく、大臣または長官の判断だけで下級庁に指示されるものですから、この解釈で課税を行う事は明らかに課税要件法定主義に反しています。更に通達でもなく解説書の一文を根拠にしたり、或いは過去の前例だけで課税をしたりという乱暴なものも見受けられます。
帰国できない高齢夫婦(三木義一)
強きを助け、弱きをくじく国税庁の姿勢を示す事例を紹介してみたい。
このご夫婦は長いこと外国で働き、外国の公的年金をもらってきたが、老後は日本で過ごしたいし、日本でも外国の年金を受領できるので帰国。ご主人が亡くなり、相続税の申告をした。すると、税務調査があり、ご主人の死亡により外国から遺族年金を受けるので、その受ける「権利」も相続財産だと言われる。年間500万円もらえる69歳の奥さんは、女性の平均余命を踏まえると、あと20年受けられるから、1億円を相続財産に加えろというのである。
実際にいくらもらえるか分からない金額に課税され、しかも、日本の遺族年金は課税されていないのにどうしてと聞くと、日本のは非課税規定があるが、外国のにはないという。そこで非課税規定を調べてみると、日本のも年金を受ける「権利」を非課税にしている
わけではなく、完全に読み間違いをしている。私も加わり、説明をすると理由を二転、三転、四転。理由がないから、課税分はやめたらと言うと、処分しないと私が処分されると言い、強引に処分をしてくるのである。
これが今、日本中でおきている。だから、外国で働いてきた高齢夫婦達は帰国できないでいる。国税庁長官か、国会議員さん、誰かが早く誤りを是正してあげないと生きて日本の土を踏めないよ!
赤井茶店
The Power and Peril of Curiosity (Christopher K. Hsee, Bowen Ruan)
Curiosity—the desire for information—underlies many human activities, from reading celebrity gossip to developing nuclear science. Curiosity is well recognized as a human blessing. Is it also a human curse? Tales about such things as Pandora’s box suggest that it is, but scientific evidence is lacking. In four controlled experiments, we demonstrated that curiosity could lead humans to expose themselves to aversive stimuli (even electric shocks) for no apparent benefits. The research suggests that humans possess an inherent desire, independent of consequentialist considerations, to resolve uncertainty; when facing something uncertain and feeling curious, they will act to resolve the uncertainty even if they expect negative consequences. This research reveals the potential perverse side of curiosity, and is particularly relevant to the current epoch, the epoch of information, and to the scientific community, a community with high curiosity.
**
Curious people do not always perform consequentialist cost-benefit analyses and may be tempted to seek the missing information even when the outcome is expectedly harmful.
On the bright side, understanding that curiosity has a dark side could help you modify your behavior and curb potentially self-destructive pursuits driven by the innate urge to close the curiosity gap. You can make better decisions if you stop and consider whether your decision making is being driven by curiosity. And, if closing the curiosity gap will have positive or negative outcomes.
Using Curiosity to Increase the Choice of Should Options (Evan Polman)
Piquing people’s curiosity can influence their choices by steering them away from tempting desires, like unhealthy foods or taking the elevator, and toward less tempting, but healthier options, such as buying more fresh produce or taking the stairs.
Evidently, people really have a need for closure when something has piqued their curiosity. They want the information that fills the curiosity gap, and they will go to great lengths to get it.
Our results suggest that using interventions based on curiosity gaps has the potential to increase participation in desired behaviors for which people often lack motivation. It also provides new evidence that curiosity-based interventions come at an incredibly small cost and could help steer people toward a variety of positive actions.
Deprivation curiosity (Jonathan Schooler)
General-interest curiosity celebrates a lack of knowledge as an opportunity to gain more knowledge. People who exhibit this trait are motivated to learn for learning’s sake. General-interest curiosity takes delight in the fact that we don’t know everything and that there’s so much wonderful information to graze out there. This expression stands in awe before mystery and accepts all that we do not—and cannot—know, which means it’s closely linked to intellectual humility.
Deprivation curiosity, on the other hand, functions in a utilitarian way. Rather than an exploratory desire to learn, it wants an answer to fill a gap in knowledge. Deprivation curiosity stems from an aversion to not knowing something; its motivation is to squelch the discomfort of uncertainty. Because deprivation curiosity clamors for information as a way to avoid unknowing, it’s linked to a lack of intellectual humility. This drive to find an answer isn’t always bad. We do think it’s likely to be an important complement to general-interest curiosity. You can easily imagine that when Einstein was pursuing his passion for understanding relativity, he had a sense of, ‘I must get to the bottom of this—I won’t sleep until I do!’
Because deprivation curiosity is linked to intellectual arrogance, it predicts other negative behaviors. When you lack intellectual humility—when you feel like you need to know everything and you realize there’s something you don’t know—that leads to an uncomfortable gap. In order to fill this gap and minimize discomfort, people tend to look for answers without discernment. For example, “we see them accepting fake news because they don’t like the feeling of uncertainty that maybe this [news] isn’t true. In a similar way, deprivation curiosity can lead people to create false memories. When we seek an answer purely to avoid not knowing, in other words, we run the risk of accepting the wrong answer.
愛と欲望(山本芳久、若松英輔)
山本 アーレントは次のように述べています。「『愛』caritasと『欲望』cupiditasは、それぞれの追求する対象によって互いに区別されるのであり、追求の仕方そのものによって区別されるのではない」。
ラテン語には愛や欲求を意味する単語が結構たくさんあります。アウグスティヌスは、それをうまく区別しながら議論を組み立てていて、caritasとcupiditasは代表的なものなんです。caritasはキリスト教的な愛ですね。それに対して欲望cupiditasとは、特にこの世的なものを自分のものにすることを意味する単語だと言います。
若松 愛と欲望について、アーレントは、愛は「善きもの」を希求すると言います。さらに愛は、「善きもの」だけでなく、永遠なるものと人間を結ぶ、とも書いています。一方で、欲望は時限的なもの、永遠ならざるものを求めていくといいますね。
山本 さらに彼女は、「人間とは、その人が追い求めるものにほかならない」とも言います。「『欲望の人』は、自らの『欲望』そのものによって消えゆく運命へと定められるが、他方『愛』は、追求される『永遠性』の故に、自ら永遠なるものとなる」とも。儚いもの、この世的なものを欲望する人は、自分自身が儚い存在であることになってしまうわけです。
欲望=クピディタスが軸になっている人は、本当に求めるべきもの、探究すべきものを見失って、その代わりに雑多な、この世的なものにとらわれる。それを「好奇心(curiositas)」とアウグスティヌスは呼びます。現代では「好奇心」はよいものと言われることが多いのですが、キリスト教哲学、アウグスティヌス以来の伝統では、「好奇心」はよからぬものなのです。
好奇心(若松英輔)
好奇心を持つのはよいことである、と教わってきた。事実、世の中は好奇心を刺激するもので満ちている。目を引く、変わった、衝撃的なものによって他者の関心を集めようとする。事実を偽り、捏造することすら試みる人たちもいる。
そのいっぽうで好奇心を強く戒める人たちがいる。哲学者のハンナ・アーレントはそのひとりだ。
Five new human rights for the Digital Age (Gerd Leonhard)
New human rights for the Digital Age
- The right to remain natural, i.e. ‘merely’ biological and organic
- The right to be inefficient if, when and where it defines our basic humanness
- The right to disconnect
- The right to be, or remain anonymous
- The right to employ or engage people instead of machines
Cassandra (ABBA)
Down in the street, they’re all singing and shouting
Staying alive though the city is dead
Hiding their shame behind hollow laughter
While you are crying alone on your bed
Pity Cassandra that no one believed you
But then again you were lost from the start
Now we must suffer and sell our secrets
Bargain, playing smart, aching in our hearts
Sorry Cassandra, I misunderstood
Now the last day is dawning
Some of us wanted, but none of us would
Listen to words of warning
But on the darkest of nights
Nobody knew how to fight
And we were caught in our sleep
Pierre Jinja (Gex)
Report on the effects of the atomic bomb at Hiroshima (ICRC archives)
Hiroshima (John Hersey)
At exactly fifteen minutes past eight in the morning, on August 6, 1945, Japanese time, at the moment when the atomic bomb flashed above Hiroshima, Miss Toshiko Sasaki, a clerk in the personnel department of the East Asia Tin Works, had just sat down at her place in the plant office and was turning her head to speak to the girl at the next desk. At that same moment, Dr. Masakazu Fujii was settling down cross-legged to read the Osaka Asahi on the porch of his private hospital, overhanging one of the seven deltaic rivers which divide Hiroshima; Mrs. Hatsuyo Nakamura, a tailor’s widow, stood by the window of her kitchen, watching a neighbor tearing down his house because it lay in the path of an air-raid-defense fire lane; Father Wilhelm Kleinsorge, a German priest of the Society of Jesus, reclined in his underwear on a cot on the top floor of his order’s three-story mission house, reading a Jesuit magazine, Stimmen der Zeit; Dr. Terufumi Sasaki, a young member of the surgical staff of the city’s large, modern Red Cross Hospital, walked along one of the hospital corridors with a blood specimen for a Wassermann test in his hand; and the Reverend Mr. Kiyoshi Tanimoto, pastor of the Hiroshima Methodist Church, paused at the door of a rich man’s house in Koi, the city’s western suburb, and prepared to unload a handcart full of things he had evacuated from town in fear of the massive B-29 raid which everyone expected Hiroshima to suffer. A hundred thousand people were killed by the atomic bomb, and these six were among the survivors. They still wonder why they lived when so many others died. Each of them counts many small items of chance or volition—a step taken in time, a decision to go indoors, catching one streetcar instead of the next—that spared him. And now each knows that in the act of survival he lived a dozen lives and saw more death than he ever thought he would see. At the time, none of them knew anything.
ロ・ギワンに会った(チョ・ヘジン)
他者の苦しみは実態が見えず、察することしかできないため、つねに何かが欠けている。
彼は希望を育む術と地の果てまで絶望する術を同時に鍛えなければならなかった。
命がけで国境を越え、最愛の人を失い、生きるためだけに見知らぬ国へと流れ着いたここまでの道のり。それが何の意味もなかったことを受けいれなければならない、氷のように冷たい時間。彼は、懐かしさだけで故郷を思い出す甘い時間は、自分には今後いっさい訪れないだろうと悟った。
生きるために生きてきただけなのに、故郷を離れて以来ずっと追われ、隠れ続けなければならない犯罪者となり、時には一人の人間として守り通したかったものまで根こそぎ奪われた理不尽な日々。
日本という異端児(立花聡)
今年は、私が日本脱出30周年。その間、アフリカのナミビアから北極のグリーンランドまで、61か国を回った。そうした中で、日本がいかに世界の異端児であるか、その本質を理解した。
異端児は問題ではない。問題は異端児であることを知らないことだ。自己中心の発想と妄想で虚構の世界を作り出し、自分の基準で行動している。自分の基準で行動することも問題ではない。ただ他に頼らず自給自足の資源が必要だ。しかし、それがない。この致命傷にも気づかない。
大方の日本人は、世界に無知であり、世界の中に存在する自分のことにはもっと無知であり、何よりも「無知の知」を持っていない。日本人は謙虚を美徳としているが、それが真っ赤な嘘。日本に対する批判に耳を傾けようとせず、相手には「反日」レッテルを貼ったりもする。
多くの日本人は日々、「日本凄い」に酔い痴れる。未だに「日本技術」を信じ込み、「日本文化」の発信に熱中する。日本は基幹産業の電機を失い、自動車産業も崩壊しつつある。そこでインバウンドの観光立国を夢見る。江戸前寿司が日本を救ってくれるとでも思っているのか。
はっきり言おう。ほとんどの外国人は日本文化に興味がない。物珍しさと安さで日本に殺到している。それだけの話。日本は、安い!物価も、不動産も、企業買収も、みんな安い。日本はバーゲン国家だ。当然、給料も安い。日本には、一旦崩壊しない限り、将来がない。30年前という早い時期に日本を脱出した自分は、いかに幸運だったか。
導いてくれた神様には、感謝、感謝、また感謝。
門(夏目漱石)
自分は門を開けて貰いに来た。けれども門番は扉の向側にいて、敲いてもついに顔さえ出してくれなかった。ただ、
「敲いても駄目だ。独りで開けて入れ」と云う声が聞えただけであった。彼はどうしたらこの門の閂を開ける事ができるかを考えた。そうしてその手段と方法を明らかに頭の中で拵えた。けれどもそれを実地に開ける力は、少しも養成する事ができなかった。したがって自分の立っている場所は、この問題を考えない昔と毫も異なるところがなかった。彼は依然として無能無力に鎖ざされた扉の前に取り残された。彼は平生自分の分別を便に生きて来た。その分別が今は彼に祟ったのを口惜く思った。そうして始から取捨も商量も容れない愚なものの一徹一図を羨んだ。もしくは信念に篤い善男善女の、知慧も忘れ思議も浮ばぬ精進の程度を崇高と仰いだ。彼自身は長く門外に佇立むべき運命をもって生れて来たものらしかった。それは是非もなかった。けれども、どうせ通れない門なら、わざわざそこまで辿りつくのが矛盾であった。彼は後を顧みた。そうしてとうていまた元の路へ引き返す勇気を有たなかった。彼は前を眺めた。前には堅固な扉がいつまでも展望を遮ぎっていた。彼は門を通る人ではなかった。また門を通らないで済む人でもなかった。要するに、彼は門の下に立ち竦んで、日の暮れるのを待つべき不幸な人であった。
Clean Meat (Paul Shapiro)
- By shifting to clean meat, we can reduce animal suffering, limit greenhouse gas emissions, conserve water, and mitigate the risks of zoonotic diseases.
- It paves the way for a more sustainable and compassionate future.
- Clean meat is not just a trend or a niche market. It has the potential to become the norm, eventually replacing conventional meat in our grocery stores and restaurants.
- The demand for meat is projected to continue rising, but our current methods of production are simply not sustainable. Clean meat offers a viable solution to feeding a growing global population without further straining our planet’s resources.
- Clean meat has the potential to revolutionize the way we produce and consume protein, addressing many of the environmental, ethical, and public health concerns associated with traditional animal agriculture.
- Imagine a world where meat is produced without the need for raising and slaughtering animals—a world where meat is clean, sustainable, and cruelty-free.
小鵬汽車(Xpeng Motors)
五十嵐博
- 臨床はラディカルになるときこそ危険である。ありふれていることが肯定されねばならない。優れた治療者とは凡庸な治療の良さを知る人なのである。
- 自分たちが持つ医学的な背景から築かれた認識や価値観よりも、患者の持つ意向や価値観をより尊重した中で、患者にとって最も望ましい方向性をともに見出していく。
- エキスパートは答えを知っているが、重要な問いを知っているのは達人だけ。エキスパートは知っていることに喜びを感じ、達人は知らないことに喜びを感じる。
- 記述することから問うことへ―客観的記述であれ、主観的記述であれ、記述することは問うことを超えることはできない。
- 戻っていくべき本来の姿などないことを認めたうえで、「疎外」という言葉で名指すべき現象から目を背けないこと。
- 労働の廃棄でも、本来的な労働の開始でもない、労働日の短縮。
- 人はパンがなければ生きていけない。しかし、パンだけで生きるべきでもない。私たちはパンだけでなく、バラももとめよう。生きることはバラで飾られねばならない。
- 因果的な問いにデータのみで答えることは決してできない。
Slave-morality(奴隷道徳)by Nietzsche(ニーチェ)
Supposing that the abused, the oppressed, the suffering, the unemancipated, the weary, and those uncertain of themselves should moralize, what will be the common element in their moral estimates? Probably a pessimistic suspicion with regard to the entire situation of man will find expression, perhaps a condemnation of man, together with his situation. The slave has an unfavorable eye for the virtues of the powerful; he has a skepticism and distrust, a refinement of distrust of everything “good” that is there honored—he would fain persuade himself that the very happiness there is not genuine. On the other hand, those qualities which serve to alleviate the existence of sufferers are brought into prominence and flooded with light; it is here that sympathy, the kind, helping hand, the warm heart, patience, diligence, humility, and friendliness attain to honor; for here these are the most useful qualities, and almost the only means of supporting the burden of existence. Slave-morality is essentially the morality of utility.
Here is the seat of the origin of the famous antithesis “good” and “evil”:—power and dangerousness are assumed to reside in the evil, a certain dreadfulness, subtlety, and strength, which do not admit of being despised. According to slave-morality, therefore, the “evil” man arouses fear; according to master-morality, it is precisely the “good” man who arouses fear and seeks to arouse it, while the bad man is regarded as the despicable being.
The contrast attains its maximum when, in accordance with the logical consequences of slave-morality, a shade of depreciation—it may be slight and well-intentioned—at last attaches itself to the “good” man of this morality; because, according to the servile mode of thought, the good man must in any case be the safe man: he is good-natured, easily deceived, perhaps a little stupid, un bonhomme. Everywhere that slave-morality gains the ascendancy, language shows a tendency to approximate the significations of the words “good” and “stupid.”
Epictetus(エピクテトス)
If you are ever tempted to look for outside approval, realize that you have compromised your integrity. If you need a witness, be your own.
誰かに認められたいと思った時には、自分に妥協しているということに気づいてください。誰かに見てほしいと思ったら、自分に見てもらえばいいのです。
Novalis(ノヴァーリス)
Das Märchen ist der Prüfstein der Poesie … alles Poetische muss wie ein Märchen sein. Der Dichter verehrt den Zufall.
おとぎ話は詩の試金石だ…詩的なものはすべておとぎ話のようでなければならない。詩人は偶然を崇拝する。
Momo (Michael Ende)
Life holds one great but quite commonplace mystery. Though shared by each of us and known to all, seldom rates a second thought. That mystery, which most of us take for granted and never think twice about, is time.
Calendars and clocks exist to measure time, but that signifies little because we all know that an hour can seem as eternity or pass in a flash, according to how we spend it.
Time is life itself, and life resides in the human heart.
La Maison-atelier Foujita
Chevreuse
Snitching (密告)
“I was taught how to snitch by my grandfather who was a snitch himself,” claims a woman who goes by the name of Anna Korobkova. She says her grandfather was an anonymous informant for the Soviet secret police during Stalin’s reign, when denunciations were part of everyday life, and she’s following in his footsteps. Now, she is reporting anyone she thinks is a critic of the war in Ukraine.
Korobkova claims to have written 1,397 denunciations since Russia’s full-scale invasion of Ukraine. She says people have been fined, fired and labelled as foreign agents because of her denunciations.
“I do not feel sorry for them,” she reveals. “I feel joy if they are punished because of my denunciations.”
山久漆工
Stade de Reims
Rovelli’s physics: What is time? (Akira Ozeki, 3/11/2023)



すごい物理学講義 (Time doesn’t exist)
by Carlo Rovelli
書評「めぐりあう書物たち」 (Book review ”Book come across”)
by 尾関章 (Akira Ozeki)
In this column, we often cover one book over two weeks. At first, I advocated reading one book a week, but I started to think it was ridiculous to earn that many books that way. Sometimes one book every two weeks is enough. Well, sometimes it’s okay to read one book every three weeks or one book every four weeks.
So this week, I will continue with “Amazing Physics Lectures” (written by Carlo Rovelli, translated by Kaoru Takeuchi, translated by Toshihide Kurihara, published by Kawade Bunko, 2019). The reason why I linger so long on one book is because I want to get to the bottom of the loop quantum gravity theory that the author talks about, and see how the world looks.
Roughly speaking, the story of the week before last went like this. The physical world has the character of “particles”. There is a minimum unit of size, and it cannot be divided into smaller units. The microscopic world is geometric, and the way it curves can be calculated probabilistically using equations.
Last week, we looked into the nature of “particles” in the physical world. The image is like a ball packed into a box, with links between adjacent particles. It can be said to be a network-like world image. When you go around the link from particle to particle, you can see the curvature of space.
There is another feature of the space of loop quantum gravity theory that should be kept in mind. This means that it should not be seen as “an amorphous container that contains things.” The quantum of space “exists among the quanta that are adjacent to itself.” Space should be viewed as a “fabric of relationships with neighbors.”
If you review it like this, you will notice something. I wonder if this book is getting too caught up in discussing space and neglecting time. In fact, the author seems to have been concerned about this as well. In the middle of the book, at the beginning of Chapter 7, “Time Doesn’t Exist,” he frankly admits that he had not tried to discuss time until the previous chapter. However, since modern physics views time and space together as “space-time,” he declares that “it’s time to bring time back into the blueprint.”
There is also such an honest confession. Quantum gravity researchers “worked exclusively on spatial problems” until they “gathered the courage to face time.” The understanding of time has been progressing for about 15 years at the time of writing this book. Is this something that researchers have only become interested in in recent years?
Now then, what is the time image of loop quantum gravity theory? As this column has repeatedly written, the Wheeler-de Witt equation, which is the basis of loop quantum gravity theory, does not have a time variable “t”. As you read this book, you will understand what that means.
Firstly, there is a story that Galileo Galilei noticed the isochronism of the pendulum while looking at the candlesticks in the ceiling of the cathedral in Pisa. Although it seems doubtful whether this is a true story, “tradition” says that Galileo measured the period of the flickering of the candlestick by his own pulse. As a result, he realized that the period of a pendulum does not change regardless of its amplitude. The author raises the issue here. On what basis did Galileo become convinced that the pulse beats at a constant time?
There is a flip side to this. After Galileo’s discovery, doctors began using pendulums as clocks to measure patients’ pulses. He uses the pulse to check that the oscillations of the pendulum are regular, and uses the pendulum to check that the pulse is regular – that’s what we do.
The author says. Whether observing a pendulum or measuring one’s pulse, one is not measuring “time itself.” It simply measures multiple physical quantities and compares one variable with another. However, until now physics has “assumed” the existence of a time variable “t”. Quantum gravity theory breaks this custom. If we have physical quantities A, B, and C, we can define them not as functions A(t), B(t), and C(t) of “t” but as mutual functions of variables A(B), B(C), Try to think like C(A).
From this perspective, changes in the world come from changes in the relationships between things, and the world does not “change over time.” This idea is similar to viewing space not as a “container,” but as a “fabric of relationships with one’s neighbors.” It seems that time is not a “container” either.
Now, from here on it’s difficult to understand. In this column, I have no choice but to rely on the images presented in this book to proceed with the discussion. The author explains physical phenomena using “boxes.” Let’s take the example of two billiard balls colliding and rolling in two directions, and use a box to represent the time and space in which this happens. In the diagram included in this book, the box is a rectangular parallelepiped, and one side of the box appears to be a time axis, but as you read the text, you will see that this is not simply the case. This is because “the box itself “contains” space and time.”
There is another expression on the box, which makes more sense. They say it resembles a small piece of “mollusc” and is “shaped like sushi.” As an aside, there is a reason why the author brought up the term “mollusk”. This is because Albert Einstein compared the gravitational field, which is the curvature of space-time, to a “mollusk”. What made the metaphor jump to “sushi” is probably a service aimed at Japanese readers. I’m sure he himself loves Japanese food.
The question is, what is something like “sushi”? In loop quantum gravity theory, when considering the physical process of a collision between billiard balls, one must take into account not only the balls themselves, but also “everything surrounding the balls,” such as space and time. “Sushi” includes all of these.
According to this book, what we should focus on here is the end of “sushi.” One of the two ends corresponds to the beginning of the physical process, and the other corresponds to the end. The equations of loop quantum gravity theory calculate the probabilities of all possible states at the beginning and end of a process. Returning to billiards, this allows us to know probabilistically how a colliding ball enters the “sushi” and how it leaves the “sushi”. .
So, what about the space between the ends? This is where the world picture of quantum mechanics comes in handy. One is Werner Heisenberg’s matrix mechanics. “Quantum mechanics does not tell us what happens during a process,” he says. The other is Richard Feynman’s “path summation.” View the movement of particles as a bundle of paths. Based on this idea, there exists a “cloud” between the two ends that contains all possible paths that particles can take, and includes all possible space-times.
Loop quantum information theory views space as a “net.” It is said that it appears at the end of “sushi” in time and space. Now imagine the act of “holding a net in your hand and moving it”. As a result, the points of the “nodes” that are the knots of the “net” become lines, and the lines of the connections (“links”) between “nodes” become planes. The author calls this the “history of the net” and the “progress of the net,” and likens the resulting structure to a “foam.” It seems that the “clouds” in space and time can be seen as the overlapping of “all possible bubbles.”
According to this book, physicists use these “bubbles” to calculate the probability of a particular physical process. What is needed here is to add up all the “bubbles” that share the same end and find the “sum”. The equations of loop quantum theory of gravity make this calculation possible.
The time depicted in this book can be summarized as follows. There is no time or space in the world to serve as a “container” prior to an event. Space is a “net” of relationships made up of “nodes” and “links,” and “space-time” is created when the state of the “net” changes.
So why do we feel that time is flowing uniformly? This book suggests that “space and time are approximate entities that only appear on a large scale.” The “large scale” seems to have a mechanism that makes you feel the passage of time. This is explained in detail by the author in another work, and has already been introduced in this column. There is a chapter at the end of the book that will give you some hints, but for the time being I will conclude this series with three parts. Let’s take a chance and try again.
All I can say now is to stop seeing time as absolute. Time lies in the relative change of events. When I think about it, I feel like each day has become a little longer.
Rovelli’s physics: space is a web of interactions (Akira Ozeki, 27/10/2023)



すごい物理学講義 (Time doesn’t exist)
by Carlo Rovelli
書評「めぐりあう書物たち」 (Book review ”Book come across”)
by 尾関章 (Akira Ozeki)
If you continue reporting on science for a long time, you can kind of see the changes in scientists’ interests. One of the reasons is that in recent decades, more emphasis has been placed on things than things.
The reason behind this is that the elemental reductionism that colored 20th century science has reached its climax. In physics, this is the case with the rush to discover elementary particles. In the life sciences, genome decoding corresponds to this. We are approaching the limit of our ability to explore the origins of matter and life.
What emerged in its place was the science of complex systems. I’m not really interested in dividing things into smaller parts. What interests me is the relationship between things. It can also be called a network. Network theory is discussed across disciplines, from physics to biology, and from basic science to applied technology.
The trend of emphasizing networks may be related to the fact that humans themselves have become components of networks. With the spread of computers and the advancement of information technology (IT) in the latter half of the 20th century, everyone became able to connect with people around the world through the Internet. Nowadays, human society cannot exist without networks. Our thinking is connected to networks on a daily basis. Naturally, science will change as a result.
The reason why I mentioned this topic to Pillow is because I associate networks with the theory of quantum gravity in “Amazing Physics Lectures” (authored by Carlo Rovelli, supervised translation by Kaoru Takeuchi, translated by Toshihide Kurihara, published by Kawade Bunko, 2019), which I have been discussing since last week. This is because there are stories that will make you do it. Since the author considers infinitesimal space, at first glance it may seem like elemental reductionism. However, as I read further, it seems that this is not the case. Although we are assuming elements, we are looking at something network-like.
Now, let’s return to the contents of this book. Last week, this book led me to the entrance to the theory of quantum gravity, which aims to integrate quantum mechanics and general theory of relativity. It can be summarized in two points. The first point is that space is not infinitely divisible, but has a “granular” quality in extremely small areas. Another is that there is a basic equation called the Wheeler-de-Witt equation in this area, and this equation allows us to imagine space as a “cloud made up of different geometric figures overlapping each other.”
However, even if you say that, it doesn’t make sense. The fact that space is “particles” and the fact that it is “cloud-like” are not connected. I want to read this book further this week and get rid of this feeling of confusion.
Let’s start by asking whether the Wheeler-de Witt equation can be solved. According to the book, the equations were improved around the end of the 1980s, and a “strange solution” was discovered. The solution was obtained when “closed lines” (rings, loops) in space were “objected to calculation.” Another way of saying this is that a “closed line” “appears in the solution.” Apparently, loops have a special meaning. This is where the name “loop quantum gravity theory” comes from.
This doesn’t get the point across, so let’s get some help from visual materials. The book contains images of ring-like loops intertwining in all directions. If you read the text, you will see that the solution to the Wheeler-de Witt equation seems to represent the state of each loop.
The author also calls the loop the “Faraday field line of the gravitational field.” Michael Faraday (1791-1867) expressed the force of electric and magnetic fields using Faraday field lines, but this is a gravitational version of Faraday’s field lines. Since we are visualizing the state of the gravitational field, it must also be related to the curvature of space.
The points where loops touch each other are “nodes.” According to the book, these are “quantum grains of space,” or “quanta of space.” What must not be overlooked is the statement that the “volume of space” is “inside the nodes.” According to our common sense, “volume” is a continuous quantity that spreads out in space, but in quantum gravity theory it is different. “Nodes” have the character of “discrete small boxes that form a volume.” As a result, the “volume” takes on the value of Tobitobiki, and is counted as one or two.
This book also emphasizes that the “quanta of space” called “nodes” “have no place.” Since the “knots” themselves “shape the space,” they cannot locate their “place” within the space. This is very different from photons (particles of light), which are quanta of electromagnetic fields.
So, is there an alternative to the “quantum of space”? According to this book, yes. That is information about what is next to each other. Next to one “quantum of space” there is another “quantum of space”. The landscape of a space changes depending on who is next to whom.
This is the highlight of this book. “Who is next to whom?” means focusing on relationships. An image of a network comes to mind. The author’s theory of quantum gravity traces space down to the smallest particles and seems to see a web within it.
According to the author, the structure of space is made up of “nodes” that “touch each other”. At this time, a line called a “link” is assumed to connect the “nodes”. “Only through links, only in the relationships between one link and another, can individual spatial quanta be located.” The relationship between “links” also affects the “quantum of space.” I would like to note here that the author himself uses the word relationship.
By the way, from the perspective of the Wheeler-de Witt equation, a “link” can be said to be part of a loop. It can be thought of as a manifestation of the gravitational field. The gravitational field also follows quantum theory, so just as electromagnetic fields appear in the form of quanta called photons (particles of light), “links” also have quantum aspects. According to this book, this quantum is quantified by the width of the boundary surface when two nodes touch each other. Therefore, “area” also takes a value of Tobitobiki, similar to quantum theory.
The author points out that the “volume” of “nodes” and the “area” of “links” “characterize the quantum network of space.” As I read this book, I kind of realized that when we talk about what the space of the microscopic world is like, we should not imagine this space that we are currently in. There is no common sense space there. There are only “nodes”, which are particles of space, and “links” that connect them. Together with quantities such as “volume” and “area,” they form a gravitational field.
This book also includes schematic diagrams of “sections” and “links.” At first glance, they look like the vertices and edges of a polyhedron. It also resembles a diagram simulating a network such as a communication network. From this diagram, we are convinced that the latest physics, known as loop quantum gravity theory, sees networks at the root of the world.
Anyway, what exactly is a loop? This book also has some hints. The author argues that by walking the links from node to node and back, you can measure the curvature of space in one turn. This is similar to how humans measure the curvature of the Earth. For example, if you travel in a loop from the North Pole, go south, move east-west around the equator, go north, and go to the North Pole, you can detect how the Earth’s surface is curved. The loop seems to be related to spatial distortion.
Let’s summarize the story so far. In loop quantum gravity theory, the microscopic world has a granular nature. The grains of space are called “nodes.” A “node” is itself a space, so it is not in space. The location of a “section” is determined by information such as “who is next to whom.” A network of nodes and links connecting them forms the structure of the space. If you follow the “link” once, it becomes a loop, and from there you can see the curve of the space.
I see, the structure of space is like that. However, the topic of time does not come up easily. The author says that we don’t need time, but he doesn’t seem to be completely denying the flow of time. What happens to time in a microscopic world where space becomes particles? I will continue reading this book next time.
Rovelli’s physics: space is a set of particles (by Akira Ozeki, 20/10/2023)



すごい物理学講義 (Time doesn’t exist)
by Carlo Rovelli
書評「めぐりあう書物たち」 (Book review ”Book come across”)
by 尾関章 (Akira Ozeki)
Recently, this column has been confronting the mystery of time. The reason is probably because I’m older. Every day is so precious. To put it more simply, I love every moment. However, you cannot capture that moment and save it somewhere. There is no cryopreservation in time.
In May of this year, I read “Time Doesn’t Exist” by theoretical physicist Carlo Rovelli (translated by Sei Tominaga, published by NHK Publishing, 2019). The emphasis was on the fact that physics can work without time. Physical phenomena can be described without the time variable “t”. If you use mathematical formulas to relate the way one quantity changes to the way another quantity changes, you can accomplish the mission of physics – it’s surprising when you think back to science class, but it was a point that made sense once you heard it. .
However, this cannot explain how we experience time every day. What makes “Time Does Not Exist” admirable as a book for the general public is that it does not ignore its drawbacks. The author, Rovelli, used thermodynamic considerations to reveal the true nature of time as we humans perceive it.
However, since I was a science reporter, I would like to take a step closer to Rovelli’s physics, which says that there is no need for time. What kind of philosophy did he draw from? How is he trying to change his worldview? There are many things I want to dig into. So this time I will be looking at another book by the same author. Coincidentally, this column, including its predecessor column, has now reached its 700th anniversary. I once had a sign saying “Bunri Yuyu” in the name of my column, so I think it’s a fitting choice for this milestone.
“Amazing Physics Lecture” (written by Carlo Rovelli, translated by Kaoru Takeuchi, translated by Toshihide Kurihara, Kawade Bunko, published in 2019). This is a paperback version of the Japanese translation published by Kawade Shobo Shinsha in 2017. The original book was published in Italy in 2014, three years earlier than the original publication of “Time Doesn’t Exist.”
The author is from Italy. He is searching for a theory that integrates quantum mechanics and general relativity, and advocates the “loop quantum gravity theory” as a trump card. This theory is tied to cosmology and is deeply concerned with what happened at the beginning of the universe. This is one of the reasons why I am trying to read this author’s book again. If time does not exist in physics, as “time does not exist” says, then what was the origin of the universe? I would like to get that hint as well.
Let’s get into the contents of this book. Chapter 1, “Grains: The Great Discovery of Ancient Greece” states, “The universe is granular and does not continue smoothly.” Its origin seems to be the atomic theory of the ancient Greek philosopher Democritus. The idea is that the work of cutting the universe into pieces cannot continue indefinitely, and this has the advantage of resolving Zeno’s paradox that the hero Achilles cannot catch up with the tortoise. As you read this book, you will find that the author also takes the position of Democritus.
This is where the word “granularity” comes from. The author says that “at the root of all things” is “the nature of particles.” Quantum theory considers that electromagnetic waves are also swarms of photons (particles of light), but quantum gravity theory seems to believe that space and time also have “granularity.”
This book cites former Soviet physicist Matvey Bronstein (1906-1938) as a pioneer in this research. He viewed space as a “continuum that can be infinitely divided” and published a paper in the 1930s that showed that quantum mechanics and general relativity were incompatible. He theoretically proved that if quantum mechanics and general relativity are both correct, space has a “granular” quality. This man was sentenced to death for criticizing the Stalinist regime in the former Soviet Union, and was executed at a young age.
This is how the proof works. If you try to place a particle in a very small region of space, that particle will follow Heisenberg’s uncertainty principle and try to escape from that region at extremely high speed. The energy of the particles becomes enormous. According to general relativity, the result is that space bends so much that its interior becomes unobservable. In modern terms, this creates a black hole. It can be said that “areas below a certain scale” are “inaccessible” and therefore nothing exists there.
Bronstein calculated that “certain scale”. This can be obtained by multiplying Planck’s constant h by Newton’s gravitational constant G, dividing it by the cube of the speed of light c, and taking the square root of the result. It will be done. h is a fundamental constant related to the discrete values of energy in quantum theory. c is a constant essential to relativity theory. A calculation formula that includes both is suitable for attempting to reconcile quantum mechanics and general relativity. The value thus obtained was the “minimum length” that exists in the world.
This length is 1 trillionth of 1 trillionth of 1 cm (10 to the minus 33rd power cm). The physics community has named this the “Planck length,” but the author says, “I would like to call it the “Bronstein length.” This is probably a tribute to the pioneers of quantum gravity theory.
John Wheeler (1911-2008), a prominent American physicist, made a major contribution to the development of quantum gravity theory. It is said that it was because of this person’s intention that a celestial body that collapses due to gravity came to be called a black hole. According to the book, Wheeler was able to visualize quantum space in a single image after carefully reading Bronstein’s paper. It was “a cloud-like thing made of different geometric figures overlapping each other.”
Speaking of “cloud”, the electron cloud of quantum mechanics comes to mind. When we consider the electrons around the atomic nucleus using Schrödinger’s equation, they do not exist at a single point unless they are observed, but instead exist in a series of overlapping states at various positions. It is a “cloud of probability.” According to the theory of quantum gravity, does this mean that space is similar? However, it is not the positions of the electrons that overlap, but the shapes of the geometric figures. I feel like I understand something, but this alone doesn’t make sense.
The author compares this to the sea level. If you look at the ocean from above, it looks like a flat, blue plate, but if you get closer, you’ll see bubbles floating here and there. When viewed macroscopically, space is “flat and smooth” and follows Euclidean geometry, but this is not the case with microscopic scenery.
For example, suppose we look into a world where the scale of a ruler is as small as Planck’s length. Space is there “chopped and bubbling.” The book explains that this “bubbling of space” is “a wave of probability made up of different geometric figures.”
What was brave about Wheeler was that he attempted to describe the “bubbling of space” using a mathematical formula. He was collaborating with a young researcher, Brice de Wit. In the 1960s, the two discovered the “Wheeler-de Witt equation.” It was estimated that the probability of observing a particular curved space could be determined from this formula. If successful, it will be a quantum gravity theory version of Schrödinger’s equation that gives the probability that a particular particle state will be observed.
So, did you solve the Wheeler-de Witt equation as expected? I’d like to go into that, but I’ve run out of lines this week. I’ll be taking up this book again next week and talking about it.
This time, I would like to add one more thing about the Wheeler-de Witt equation. In “Time Doesn’t Exist,” the author described this formula as “pointing out possible relationships between varying quantities without involving the time variable.” This book says the same thing.
According to modern cosmology, the universe began in an ultra-microscopic world. According to quantum gravity theory, the author’s position seems to be that it can be drawn without the time variable “t”. The world became what it is today due to rapid expansion (inflation) or a big explosion (big bang).
What I would like to mention here is Stephen W. Hawking’s theory. It is said that there was an imaginary amount of time at the beginning of the universe. At this time, “Time and space may come together to form a curved surface of finite size but without any boundaries or edges.” (“Hawking talks about the universe: From the Big Bang to black holes.” “Until” (written by Stephen W. Hawking, translated by Kazu Hayashi, Hayakawa Bunko NF). Is it impossible to distinguish between time and space?
Whether you accept the Wheeler-de Witt equation or support Hawking’s cosmology, it seems that when thinking about the beginning of the universe, you should put time aside and focus on space for now. The question is, what is the space like? That’s what we’ll focus on next week.
Physics that allows us to feel the flow of time (by Akira Ozeki, 12/5/2023)



時間は存在しない (Time doesn’t exist)
by Carlo Rovelli
書評「めぐりあう書物たち」 (Book review ”Book come across”)
by 尾関章 (Akira Ozeki)
Last week, I talked about how physics doesn’t require time. The book he read was “Time Doesn’t Exist” (written by Carlo Rovelli, translated by Sei Tominaga, published by NHK Publishing in 2019). Since it was written by a theoretical physicist, it cannot be dismissed as some sort of nonsense. At least I was satisfied.
The heart was something like this. When things change, we describe the change as a function of the time variable t. “T” is like the hands of a clock. In other words, in our daily lives, we relate changes in things to changes in the clock.
However, the author argues that the person to be associated does not have to be a watch. It does not have to be a guideline for a day, month, or year like the rotation of the Earth, the revolution of the Moon, or the revolution of the Earth. If you relate one change to another change, you can create a physical equation.
I see. In that case, it may be safe to say that “time does not exist.” But there’s a trick here. It is hidden in the word “change”. When we say things change, we think of time. Getting rid of “t” does not mean getting rid of time.
Let us recall philosopher John Ellis McTaggart’s theory of time, which we discussed in this column the other day. This also referred to the “unreality of time.” However, in the process of proving this, he also taught me that there is an aspect of time that cannot be expressed with the letter “t”.
According to McTaggart, time can be divided into three series: A, B, and C. Both series A and B are important; series A focuses on the “distinction between past, present, and future,” and series B focuses on “the distinction between earlier and later.” Neither of these two points of view can fit within the “t” frame.
As for the A series, in this world a change is occurring in which future events turn into present events, and then eventually become past events. This change cannot be explained only by the time axis representing “t”. On the other hand, the B series is a bit more complicated. “Before and after” are easy to fit into the image of a time axis. However, why do we view the negative direction as “before” and the positive direction as “later”? There is something about time that cannot be measured by the number of “t”s.
What we can say from the above is that although the world exists without the time variable “t”, we still recognize that there is time in the world. This is another theme of this book, “Time Doesn’t Exist,” and is explained in detail later in the book. This week, let’s focus on that.
The keyword here is “blur”. “The existence of time is deeply connected to blurring,” the author declares, “blurring occurs because we are unaware of the microscopic details of this world.” He says that time is nothing but a manifestation of human ignorance.
When I hear this story, people like me, who studied physics in my student days, feel like I understand that he is talking about entropy. Entropy is a numerical value that appears in thermodynamics and statistical mechanics. I remember that in the lecture, it was explained as “the total amount of information that has been lost.”
Let’s take a glass of water as an example. What we are looking at is the “macroscopic state” of liquid water in a transparent container. There are countless water molecules in water, each in a variety of positions that are difficult to distinguish. This blurring is entropy. The author explains that the value of entropy is determined by the number of configurations that are indistinguishable to us, based on the theory of Austrian physicist Ludwig Boltzmann.
In physics, there is a “law of increasing entropy” (the second law of thermodynamics), which states that entropy only increases. It refers to a situation where the documents stacked neatly on a desk suddenly turn into a pile of disorganized paper. There, an “orderly arrangement” changes to a “chaotic arrangement.” This is not just about paper documents. The author sees the state of the universe as “a gradual process of disorder, like a deck of cards being shuffled out of order.”
What is interesting is that this book uses entropy to explain the difference between the past and the future. According to the author, the past “leaves its traces in the present.” Craters on the moon, fossils of ancient creatures, and memories in the brain are nothing but such “traces.” So, why are there traces of the past but no traces of the future? According to the authors, this is due to “low entropy in the past.” He says he cannot find anything else that “creates the difference between the past and the future.”
I wonder if it’s true. This seems to be related to the law of conservation of energy. Traces are created when something stops moving and kinetic energy turns into thermal energy, like when a meteorite hits the moon and creates a crater. Since the change to heat is disordered, it progresses over time. In this way, the traces can be seen after the fact. Future events will also leave traces, but they cannot be confirmed in advance at the present moment.
According to the author, the reason we feel that the past is “fixed” is because there are many traces. As a result, the brain develops an “extensive map of past events,” and is bound to that past. In contrast, in the future, there are no visible traces, so there are many options.
Now that we’ve come this far, let’s review last week’s story again. According to this book, the world is made up of a network of events. Therefore, it can be described by the relationships between many variables. In fact, this week’s story is not unrelated to this world image.
According to this book, we “belong” to “parts” of the world. What it means to be a part is that the variables that interact with us are not all variables. It is a position that believes that humans are not concerned with the world as a whole, but only with a part of it.
This affects entropy. Entropy reflects the degree of “blurring,” but the degree of blurring depends on “which variables we interact with.” “Which variables interact with” differs from part to part, so the degree of “blurring” also depends on the part to which you belong. So where are we humans? The authors explain that the images are placed in areas where “entropy when the world began” “appears to have been extremely low.”
The author understands the state of low entropy in the early universe as follows. “The universe is not arranged in a special way.” “We belong to a special physical system, and the state of the universe related to that physical system is special.” – Here, “physical system” refers to It’s about the parts.
I think this view is closely related to the anthropic principle of cosmology. The anthropic principle holds that the universe is the way it is because otherwise humans could not exist. The author’s view of time is similar to this, and seems to be saying that the reason why time flows in this way in the universe is because humans would not be able to sense time otherwise. You could say that we happen to be in a part of the universe where time flows like this.
There is one more thing I would like to add about “parts”. The author connects the meaning of “perspective” to “interacting with a small portion of the countless variables in the universe.” Since we see the universe “from within,” we cannot describe the world without a “perspective.” What cannot be ignored are words such as “now,” “here,” and “me,” which change their designation depending on the situation…This thesis reminded me of McTaggart’s theory of time.
The translator’s “Appendix” to “The Unreality of Time” (written by John Ellis McTaggart, translated by Hitoshi Nagai, commentary and commentary, Kodansha Academic Library) is associated with “the simple present” and “the simple self” It was done. Whether you’re a philosopher or a physicist, is it essential to have an inside perspective when talking about time?
After reading this book, “Time Doesn’t Exist,” I realized that the image of time in the sciences and humanities has gotten much closer in recent years. However, there is still a wall between the two that must be overcome. For example, how does “trace” relate to the “distinction between past, present, and future” in McTaggart’s theory of time? Or, how does the “change” in which the future becomes the present and eventually reaches the past relate to an increase in entropy? There are so many questions I want to ask. I want to continue to think more slowly about time.
“Time is not there” said the physicist (by Akira Ozeki, 5/5/2023)



時間は存在しない (Time doesn’t exist)
by Carlo Rovelli
書評「めぐりあう書物たち」 (Book review ”Book come across”)
by 尾関章 (Akira Ozeki)
Looking at the roses, I think that early summer has arrived again. Time passes quickly as you get older. Sometimes the end of time flickers in my head as I realize that life is finite. Time is a real concern. This spring, this column read philosopher John Ellis McTaggart’s theory of time.
However, philosophy discussions only cover half the time. There is a group of people in academia who think of time from a completely different perspective. Natural scientists, especially physicists.
The natural world is made up of objects. Objects are positioned using coordinates on the spatial and temporal axes, and their movement can be described by speed, which is the change in position in space divided by time, and acceleration, which is the change in speed divided by time. We have become accustomed to seeing things that way. In modern times, the limits of Newtonian mechanics have become apparent, and complicated topics such as the theory of relativity and quantum mechanics have emerged, but the general framework of space and time appears to be intact.
As I wrote in the previous article, the time picture for liberal arts students is not straightforward, but the time picture for science majors has a good outlook. “Where is Time Born?” (written by Junichiro Hashimoto, published by Shueisha Shinsho, 2006), which was previously featured in “Book Reading by Chance”, was able to see through this rupture in literature and science.
Mr. Hashimoto pointed out this. “The theory of time expounded by modern philosophers almost completely ignores the nature of time revealed by modern physics (mainly relativity and quantum theory)” “On the other hand, the theory of time expounded by scientists is based on the framework of science.” It never comes out. It never tries to enter human time.” I feel the same way. It’s strange that even scientists can be busy or relaxed. Recently, however, people in the field of physics have begun to step into “human time.” It’s not just Mr. Hashimoto.
“Time does not exist” (written by Carlo Rovelli, translated by Sei Tominaga, published by NHK Publishing, 2019). I learned about this book in the newspaper when it was first published (Asahi Shimbun November 16, 2019, morning edition reading page, “Selling books” column). The reviewer is Takumi Fukuo, a critic. “This book is engraved with an intellect that goes beyond the easy division between liberal arts and science majors, or rather, the appeal of the humanities that can only be brought out by science majors,” he concluded. I thought the same thing when I read it. It’s no wonder that the book’s belt reads “Revolutionary Theory of Time.”
The author is a physicist born in Italy in 1956. After receiving his PhD from the Graduate School of the University of Padua, he continued his theoretical research at universities in Italy, the United States, and France. He is trying to construct a theory that combines the theory of relativity and quantum mechanics, and is one of the advocates of the “loop theory of quantum gravity.” Meanwhile, he has also written a series of physics books for the general public. This book was published in Italy in 2017. According to the author’s introduction, it has been published in over 30 countries and has become a “global bestseller.”
There are two main points in this book. The first is that physics can be done without time. The other thing is that we still feel like we have time. The latter concerns human nature. Because of the second reason, we can say that we are stepping into “human time.”
Many science fans already know that time is not absolute. This is because in the 20th century, Albert Einstein established the theory of relativity, which refuted the absolute time theory of Isaac Newton’s physics. This book also emphasizes this.
For example, at the beginning of Chapter 1, “Time changes when you change places,” it is written that “Time flows faster in the mountains and slower in the lowlands.” This is an effect of general relativity. He explains that “objects slow down time around them,” and that “the degree of deceleration is greater in flatlands than in mountains because flatlands are closer to the Earth’s center of mass. ” (Translation notes are in brackets, and bold text follows the original text.) I was perplexed by the way this story started, and then I understood it. This person is clever!
General science books that deal with Einstein’s theory of relativity usually begin with special relativity. Special relativity is a theory that deals with inertial coordinate systems, so it can be considered with an easy-to-understand image of a train and a station platform. In fact, Einstein himself first completed his special theory of relativity and then moved on to general relativity. However, the author suddenly presented general relativity to the reader. My guess is that this is because he wanted to impress that time is related to “objects.”
There is a brilliant argument in the explanation of general relativity. This is how the gravity works between the sun and the earth. “Rather than being directly attracted to each other, I think they each act on things in between.” This is the so-called proximity effect. If that’s the case, then “the sun and the earth should be causing changes in the time and space around them, just as an object submerged in water displaces the water around it.” If space-time is a transmitter of gravity, then it is a concrete block. It cannot be a rigid body like .
In the story so far, time exists. However, it is influenced by objects. To this extent, the author emphasizes objects rather than time. However, if you read it carefully, you will see that the object is not seen as absolute either. In fact, it’s the opposite. He sees objects as illusions.
This story appears in Chapter 6, “This world is made of events, not things.” He fully develops a worldview that values things more than things. He uses the example of a stone, a representative object, to make this statement. It is “a process in which it is possible to maintain its shape and balance for a very short period of time before it collapses and returns to sand.” Both classical and modern physics talk about “the way events occur,” rather than “the state of things,” and they say that “things” are nothing more than events that do not change for a while.
Based on this way of thinking, the world is a “collection of events.” Moreover, they are interconnected and form a “network of events.” Physicists have long searched for the “identity of fundamental entities” through particle research, but recently they have discovered that it is easier to understand the world by understanding the “relationships between events.” A worldview that values things over things can be rephrased as a worldview that values “relationships” over “substances.”
The author also talks about humans using the theory of “networks of events.” Human beings themselves are events that involve “complex processes in which food, information, light, words, etc. enter and exit,” but they also involve “social relationships,” “chemical reactions,” and “transactions between people of the same kind.” It becomes a “knot” in the network of “emotions” and is connected to other events. What makes this book interesting is how “food,” “light,” and “chemical reactions” are juxtaposed with “words,” “emotions,” and “social relationships.”
What cannot be overlooked is that the author views the essence of “events” as “changes.” “Events” may continue like “things,” but they only last for “a while.” Not forever. Therefore, it is better to view the world of events as “constantly changing.”
If the world is undergoing “change,” time seems to be essential. However, the author says that time is not necessary. Why is this true? This question becomes clear when we move on to Chapter 8, “Dynamics as Relationships.” We have common sense that “change” is expressed as a function of the time variable “t”, but the author does not insist on this. The way one quantity changes can be expressed in any way by relating it to the way another quantity changes. The other quantity does not have to be “t”.
Humans first related changes in things to the number of days, the phases of the moon, and the height of the sun. These gave rise to calendars and clocks, and led to “choosing one variable and giving it a special name, “time.” However, the author asserts that this is unnecessary. What I want to know is, “How do things change with respect to each other?” The basic equations of quantum gravity, which is the author’s specialty, also take the form of “pointing out possible relationships between fluctuating quantities without including time variables.”
Up to this point, I think I have gotten a vague idea of the main point of this book, which is that physics doesn’t need time. However, another difficult problem remains. Why do we feel the passage of time? I will continue reading this book next time in search of the answer to this question.
La pipe de Staline
Les gens de Vilnius l’appellent « l’appendice » ou « la péninsule ». Sur place, on préfère dire « la pipe de Staline ». Situé à 70 kilomètres au sud de la capitale lituanienne, le parc de Dieveniškes est une petite enclave en territoire biélorusse. La directrice du lycée technique du principal bourg, Ilona Sediene, entretient la mémoire de cette région occupée tour à tour par les Scandinaves, les Polonais, l’Empire russe, les nazis, puis les Soviétiques. Elle dévoile volontiers l’origine de son étonnant surnom. « Lors d’une réunion à Moscou pour dessiner les frontières de la région, Staline aurait posé sa pipe sur la carte. Personne n’ayant osé la déplacer, la ligne de démarcation a pris ici une forme arrondie. »
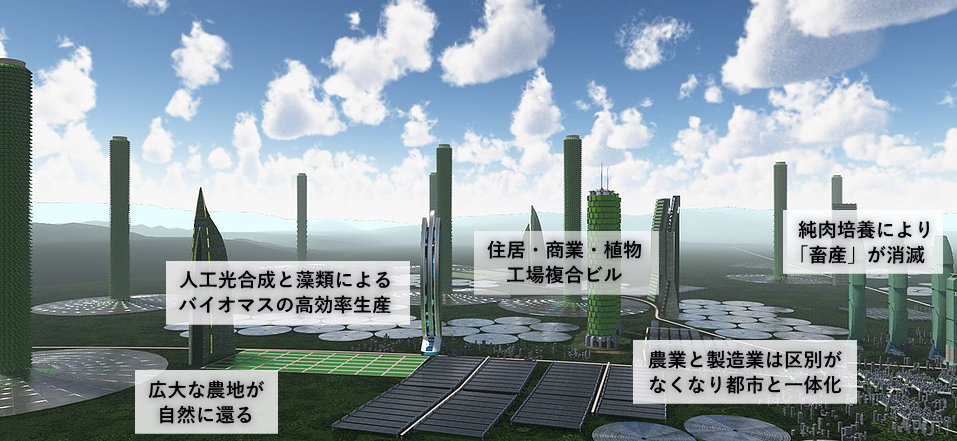
Shojinmeat
Cultured meat
In-Vitro meat is the (idea of) manufacturing of meat products through “tissue-engineering” technology. Cultured meat (= in-vitro meat = clean meat) could have financial, health, animal welfare and environmental advantages over traditional meat. The idea: To produce animal meat, but without using an animal. Starting cells are taken painlessly from live animals, they are put into a culture media where they start to proliferate and grow, independently from the animal. Theoretically, this process would be efficient enough to supply the global demand for meat. All this would happen without any genetic manipulation, i.e. without the need to interfere with the cells’ genetic sequences.
Producing cultured meat for processed meat products, such as sausages, burgers and nuggets should be comparatively simple, whereas cultured meat which should be more highly structured, such as for an in-vitro steak is considerably more of a challenge. A steak is made of muscle tissue which is threaded through with extremely long, fine capillaries which transport blood and nutrients directly to the cells. It is much more difficult to reproduce such a complex structure than it is to put together the small balls of cells which grow to larger balls of cells which in turn become in-vitro chicken nuggets.
Sébillon
Baozi (包子)
培養肉(Cultured meat)
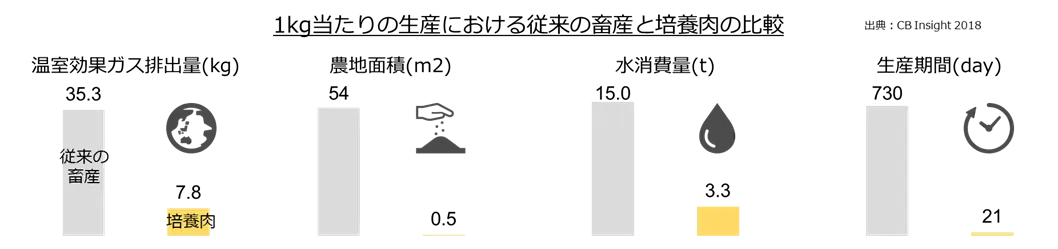
培養肉とは、「本物に近い “食肉の代用品”」のことで、英語では「Cultured meat」と呼ばれます。ウシやブタなどの動物から取り出した少量の細胞を動物の体外で人工的に培養して増やし、それらを集めて組織を作ることで生み出されます。従来の食肉生産とは違い、動物そのものが食肉の供給源にはなりません。「飼育・繁殖・解体や飼料の生産・加工などの工程」が不要となり、生産期間がおよそ2年から3週間程度へと短縮されています。
また、動物に与えるストレスや環境負荷も抑えることができます。下記は「1kg当たりの生産における従来の畜産と培養肉」を比較したものですが、①温室効果ガスの排出 ②農地面積 ③水の消費量 ④生産期間 の4カテゴリすべてにおいて「低減」が見られます。このように培養肉は動物や環境にやさしく、「クリーンミート」とも呼ばれることもあります。
Cultivated meat and seafood
Meat without killing is the central promise of what’s come to be known as cultivated meat. This isn’t a new plant-based alternative. It is, at least in theory, a few animal cells, nurtured with the right nutrients and hormones, finished with sophisticated processing techniques, and voilà: juicy burgers and seared tuna and marinated lamb chops without the side of existential worry.
It’s a vision of hedonism — but altruism, too. A way to save water, free up vast tracts of land, drastically cut planet-warming emissions, protect vulnerable species. It’s an escape hatch for humankind’s excesses. All we have to do is tie on our bibs.
Between 2016 and 2022, investors poured almost $3 billion into cultivated meat and seafood companies. Powerful venture capital and sovereign wealth funds — SoftBank, Temasek, the Qatar Investment Authority — wanted in. So did major meatpackers like Tyson, Cargill and JBS, and celebrities like Leonardo DiCaprio, Bill Gates and Richard Branson. Two of the leading companies — Eat Just and Upside Foods, both start-ups — reportedly achieved billion-dollar valuations. And today, a few products that include cultivated cells have been approved for sale in Singapore, the United States and Israel.
チベット旅行記(河口慧海)
図らざりき、私がネパールにおいて最大有力なる知己を得んとは。これまた仏陀の妙助であると感謝しました。その翌三月十日頃までは書物はこの国の図書館長が買い集めてくれますから、私は別段用事もない。それかといって余りあちこち見に歩くのも疑いを受ける種を蒔くようなものですから、殊更に司令長官に願いを出して龍樹ヶ岳に登ることを許された。龍樹ヶ岳の光景は詳しく言う必要はない。ここは龍樹菩薩の修行地また釈迦牟尼如来が因位の説法をせられた所でありまして、その説法せられた山の頂上には小さな卒塔婆が立ってあり、そこから三里ばかり降りますと龍樹菩薩の坐禅せられた窟があり、この窟で大乗仏教の妙理を観察せられたのであります。また古来の伝説に龍樹菩薩が龍宮に降って大般若の妙典を得て来たという穴はやはり岩で蓋がしてある。其穴は巌窟の少し東の山間にあるので、即ち尸棄仏陀の塔の横に在る家の中に在るのですが、この穴は十二年に一遍ずつしか開けられない。
そもそも龍樹菩薩は大般若経の妙理について、如来の説かれた小さな原本によってその説を敷衍するためこの窟に坐禅せられたので、その坐禅の有様を形容して龍宮に入ったというのか、あるいはまたその外に宗教上不可知的の真理があって坐禅の上であるいは他の世界の仏典を得て来たのか、これは未定の問題でありますけれども、大乗は釈迦牟尼如来の説かれたものであるということはチベット語にて伝わって居る龍樹菩薩の伝記によっても分ることであります。
で龍樹ヶ岳から帰りましてその夜は龍樹ヶ岳に登るの賦を作り、それから真妙純愛観ならびに雪山にて亡き父を弔い、在せる母を懐うというような歌を作るのを仕事にして三月十日頃まで過ごしました。こういう事でもしなければ外にどうもしてみようがない。地理や何かの取調べをすれば直に疑いを受けます。私は何も疑いを起されてまでその国情を取調べにゃあならぬという必要はないから、まあ自分の好きな仕事をして居りました。
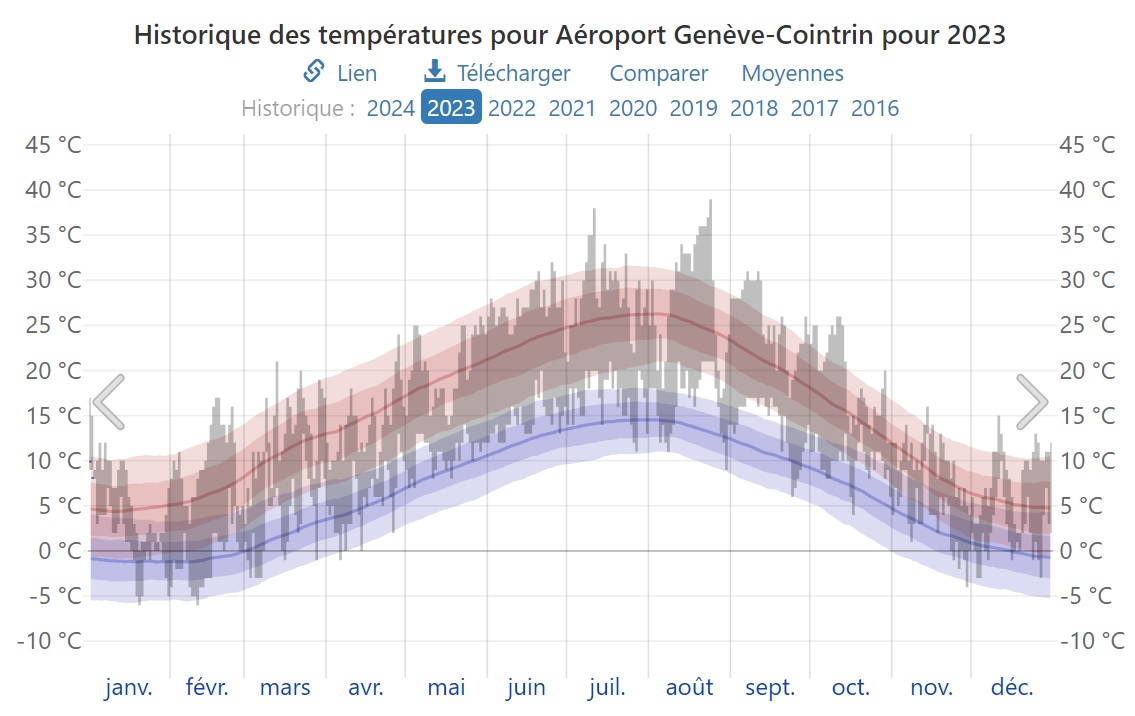
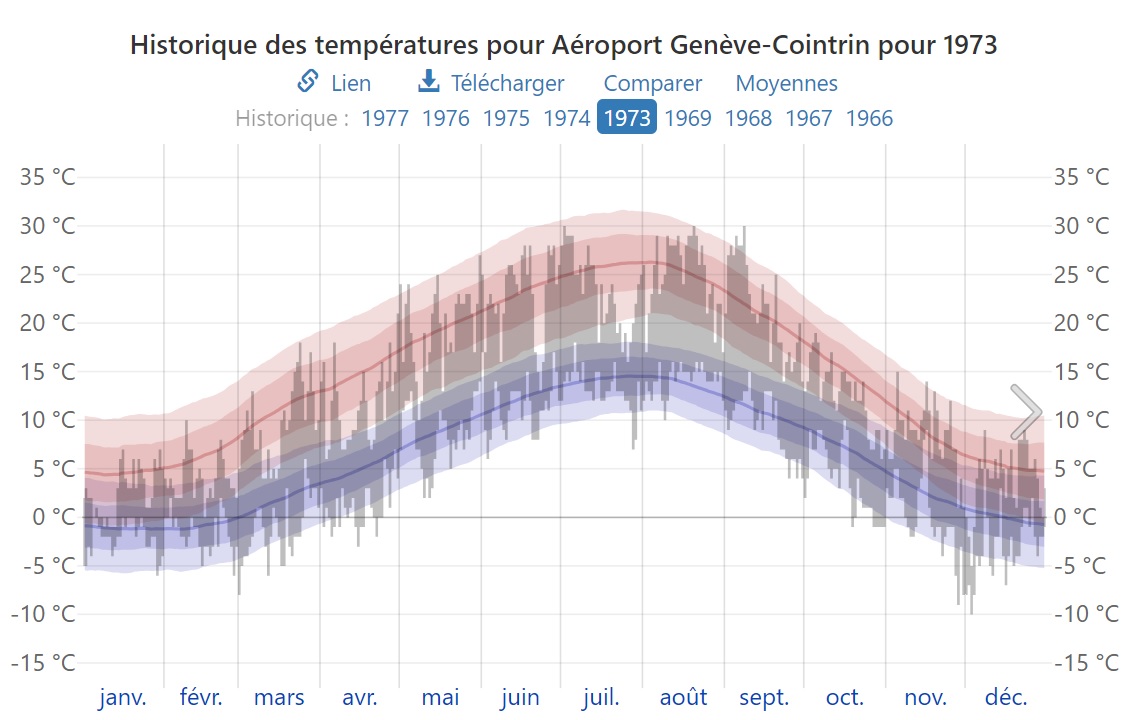
Températures
湖州師範学院 サステイナビリティ研究院(松下和夫)
 湖州師範学院には「両山」理念に基づき、学際的かつ総合的共同研究を実施するイノベーション創出機関である「サステイナビリティ研究院」が設立されています。
湖州師範学院には「両山」理念に基づき、学際的かつ総合的共同研究を実施するイノベーション創出機関である「サステイナビリティ研究院」が設立されています。
「両山」理念とは、2005年に当時中国共産党浙江省党委員会書記を務めていた習近平氏が、浙江省の安吉余村を実地調査した際に、「澄んだ水と青い山こそが金山であり銀山である」(緑水青山就是金山銀山)との理念を提唱したことが起源とされています。実際この「両山」理念のスローガンは、地域のいたるところに掲げられています。
湖州師範学院のサステイナビリティ研究院は、この理念を持続可能な発展と結び付ける具体的な研究を進めています。その具体的な例が「持続可能な竹の活用」です。両山理念の発祥の地、浙江省安吉余村は豊富な竹林に覆われています。竹は成長が早く、持続的に活用が可能な植物資源です。日本や中国など東アジアには多くの竹林があり、旺盛に生い茂っていることから、その有意義な活用を提起することは重要です。しかし、中国でも近代化の進行に伴い、多くの竹製品が姿を消そうとしています。安吉余村では湖州師範学院と連携し、「竹をもってプラスチックを代替しよう」(以竹代塑)とのスローガンで、様々な製品を開発し、その展示館(安吉优品)を設けています。
永瀬正敏
南野拓実(Takumi Minamino)
Content democratization (Adobe)
As the name implies, content democratization allows individuals and small businesses to create and share digital content in more ways than would have been possible in the past. It eliminates previous limitations of the traditional media space, such as price and technology barriers that restricted content creation and sharing to fewer people.
This new media may include blogs, ebooks, podcasts, songs, videos and other digital content. It’s often supported by online platforms such as YouTube, TikTok, Facebook, Instagram, Snapchat or LinkedIn, which allow users to distribute content at little or no cost. As a result, the creative industry is changing rapidly and the boundaries between old media and new media are evolving.
Democratization of music creation
The integration of AI into various creative tools is inevitable. AI is already influencing image generation and music creation will follow suit. Tools used for video creation and digital audio workstations will also incorporate AI features, improving user accessibility and enhancing the output.
Such advancements will provide an avenue for countless individuals who have a passion for music but might not possess the technical skills. It’s an opportunity for them to express their creativity. This is a significant move in the music industry, mirroring the transformation brought about by streaming services. These platforms, such as Spotify and Soundcloud, have made music distribution accessible to everyone. As a result, a vast number of songs are being uploaded daily.
A third of art galleries do not expect to survive
A recent survey conducted by The Art Newspaper discovered that as a result of global lockdown, art galleries around the world are expected to lose an average of 72% of their annual revenue. The survey of over 236 international dealerships revealed that the drop in financial activity ranges from region to region with UK galleries suffering the highest loss at 79% and with European at the opposite end with 66%.
Of even greater concern is the fact that approximately 30% of gallery owners believe they will not survive the crisis. With the smallest galleries, those with between 5-9 employees, predicted to have the lowest chance of survival at just 62%. Larger galleries have a rather more optimistic outlook and have put their chances of survival at 75%.
Generative AI’s impact on creative work (Ziv Epstein)
Generative AI tools are doing things that even a few years ago we never thought would be possible. This raises a lot of fundamental questions about the creative process and the human’s role in creative production. Are we going to get automated out of jobs? How are we going to preserve the human aspect of creativity with all of these new technologies?
The complexity of black-box AI systems can make it hard for researchers and the broader public to understand what’s happening under the hood, and what the impacts of these tools on society will be. Many discussions about AI anthropomorphize the technology, implicitly suggesting these systems exhibit human-like intent, agency, or self-awareness. Even the term “artificial intelligence” reinforces these beliefs: ChatGPT uses first-person pronouns, and we say AIs “hallucinate.” These agentic roles we give AIs can undermine the credit to creators whose labor underlies the system’s outputs, and can deflect responsibility from the developers and decision makers when the systems cause harm.
Labastide-d’Armagnac
文学部の終わり(by アザラシさん)
今の日本の大学生は勉強しません。本当に、びっくりするくらいしません。大人も似たようなもんですが。
学部のレベルでは、文学を研究する、と言っても、研究なんてとても言えたものじゃありません。例えば、授業でこの文学を研究しましょう、となって教授から「研究」を求められても、大学生はポンコツなので、ただの「読書」をして、「感想」を書いています。論文なんて、書ける人ほとんどいません。
就職活動の面接で、難しいことを難しいまま言ってもネガティブチェックに引っかかって落ちるだけです。難しいことを簡潔に話せないと落ちますし、それができたら優秀だなと思われて採用される可能性が高くなることもあります。
なので、本当の意味で文学を研究している人は、難しい言葉を難しい言葉のまま使っていると思います。でもそれは、私の関心事である、就職活動とか、ビジネスでは排除しないといけないものなので。
人生に深みをもたせたり、人を豊かにするのは文学の「研究」が大切なのは分かります。
でもビジネスが、会社が、資本主義が、経済が、周りの人間が、難しい言葉を嫌うんです。
私は文学好きですし、信念とか哲学とかを考えるのは大好きです。でもそういうのって世の中では少数派っぽいですし、何と言うかそういう空気を感じて、この感情は周囲に対して全面的に出せません。
侘助椿(薄田泣菫)
「この花には捨てがたい侘があるから。」
かういつて、同じ季節の草木のなかから侘助椿を選んで、草庵の茶の花とした茶人の感覚は、確かに人並すぐれて細かなところがあつた。壁と障子とに仕切られた四畳半の小さな室は、茶人がその簡素な趣味生活の享楽を一盌の茶とともに飽喫しようとするには、努めて壁と障子との一重外に限りもなく拡がつてゐる大きな世間といふものを忘れて、すべて幻想と聯想とを、しつかりとこの小天地の別箇の生活のうちに繋いでゐなければならぬ。
それには生活の方式がある。その方式といふのは、長い間かかつて磨かれた簡素な象徴的なもので、例へば、釜の蓋の置き場所から、茶杓の柄の持ち方に到るまで、きちんと方式が定まつてゐて、それを定められた通りに再現することによつて、方式それみづからの持つ不思議な力は、壺のやうに小さな茶室に有り余るほどゆつたりとした余裕と沈静とを与へ、そこにゐる主客いづれもの気持に律動と諧調とを生みつけ、また日ごとにめまぐるしくなりゆく現実の生活とは異つた、閑寂と侘とのひそやかな世界を皆のうちに創造しようとする。
そのひそやかな世界では、床の間に懸つた古い禅僧の法語の軸物、あられ釜、古渡りの茶入、楽茶盌、茶杓、――といつたやうな道具が、まるで魔法使の家の小さな動物たちが、主人の老女の持つ銀色の指揮杖の動くがままに跳ねたり躍つたりするやうに、それぞれの用に役立ちながら、みんな一緒になつて茶室になくてはならない、大切な雰囲気をそこに造り上げようとする。大切な雰囲気とはいふまでもなく、閑寂と侘とのそれである。
むかし、小堀孤蓬庵が愛玩したといふ古瀬戸の茶入「伊予簾」を、その子の権十郎が見て、
「その形、たとへば編笠といふものに似て、物ふりてわびし。それ故に古歌をもつて、
あふことはまばらにあめる伊予簾
いよいよ我をわびさするかな
我おろかなるながめにも、これをおもふに忽然としてわびしき姿あり。また寂莫たり」
といつたのも、その茶入が見るから閑寂な侘しい気持を、煙のやうに人の心に吹き込まないではおかなかつたのを嘆賞したものなのだ。
もしか茶室の雰囲気に少しでももの足りなく感じたら、そんな場合には何をおいても床の間の抛入の侘助の花を見ることだ。自然がその内ぶところに秘めてゐる孤独感が、をりからの朝寒夜寒に凝り固まつて咲いたらしい、この花の持味は、自然の使者として、その閑寂と侘心とを草庵にもたらすのに充分なものがあらう。
私は暗くなつた室でこんなことを思つてゐた。椿の花は小さく灰色にうるんで、闇の中に浮き残つてゐた。
China (Koreans’ top overseas direct shopping destination)
Armed with low-cost products, China has stepped up as Koreans’ top overseas direct purchase destination last year, overtaking the U.S.
Koreans spent a total of 6.75 trillion won ($5.08 billion) in direct purchases of overseas products online throughout the past year, a 26.9 percent jump from the previous year.
By countries, the overseas direct purchase market last year was driven mainly by China, which has several mega-sized online shopping malls, including AliExpress and Temu, to attract Koreans with their low-cost products and pervasive online promotions.
Out of the aggregated 6.75 trillion won that Koreans spent on overseas direct purchases, China accounted for 3.28 trillion won, or about 48 percent, posting a whopping 121.2 percent surge compared to the previous year.
The U.S., which had held the top position as Koreans’ most favored overseas direct purchase destination, saw its ranking drop to second place. The U.S. took up 1.85 trillion won of the annual transactions, or 27 percent, down by 7.3 percent compared to the year before.
Cosette balayant (Émile Bayard)
Mu Cang Chai
SUV à Paris : faut-il en finir avec les grosses voitures ?
A Sad, Lonely, Angry and Mean Society (David Brooks)
I’d argue that we have become so sad, lonely, angry and mean as a society in part because so many people have not been taught or don’t bother practicing to enter sympathetically into the minds of their fellow human beings. We’re overpoliticized while growing increasingly undermoralized, underspiritualized, undercultured.
The alternative is to rediscover the humanist code. It is based on the idea that unless you immerse yourself in the humanities, you may never confront the most important question: How should I live my life?
Chemin de Compostelle (Saint Jean Pied de Port)
Maison Chrestia à Orthez et Eyhartzea à Hasparren (Francis Jammes)
日本の人口(国土交通省)
Gabriel Attal et Jordan Bardella
Junya Ito (Brigitte Macron, Didier Deschamps)

 Brigitte Macron: Il y a un Japonais qui joue très bien à Reims. Comment s’appelle-t-il déjà ?
Brigitte Macron: Il y a un Japonais qui joue très bien à Reims. Comment s’appelle-t-il déjà ?
Un journaliste: Junya Ito ?
Brigitte Macron: Oui, Ito c’est ça. Il est très bon. Il faut le sélectionner dans l’équipe Didier ! Pourquoi vous ne le prenez pas ?
Didier Deschamps: Bah parce qu’il est Japonais.
Tyranny of majority(熊谷 晶子)
トクヴィルは民主主義の欠点として「多数者の専制権力(tyranny of majority)」を指摘している。彼は「多数者の支配が絶対的であるということが、民主的政治の本質」であるといい、多数者の前には何者も無力で、少数派の声に耳を傾ける余裕も感じられないような事態は危険だと忠告している。世論が多数者を作り出す。立法団体も多数者を代表してこれに盲従している。執行権力も多数者によって任命される。警察は武装した多数者であり、陪臣は逮捕を先刻する権利を与えられている多数者、さらに判事たち自身も一部の州では多数者によって選ばれているという状況では、少数派は不条理に遭遇しても誰にも訴えられない。実際トクヴィルはこのような「圧制」が頻繁にアメリカで行われていたといっているのではなく、そのような「圧制」を防止する保障がないことを危険視していた。
浅原六朗の晩年の弟子の歌
より添って眠り
温めあって起きる
穏やかけき
春夏秋冬
Impact of AI (Varun Srinivasan)
Since late 2022, the prevalence and influence of generative AI technologies have significantly increased across a range of industries, including higher education. The implications of generative AI are particularly complex and multifaceted in the context of college admissions, where the authenticity and uniqueness of student applications are crucial.
Admissions officers’ traditional metrics and methods for assessing applicants’ originality and personal voice are coming under pressure as AI tools get more sophisticated at producing creative content, from essays to artistic works. Over time, educational institutions might need to pivot to new methods to maintain the objectivity and fairness of their selection standards.
Democracy (Alexis de Tocqueville)
I seek to trace the novel features under which despotism may appear in the world. The first thing that strikes the observation is an innumerable multitude of men, all equal and alike, incessantly endeavoring to procure the petty and paltry pleasures with which they glut their lives. Each of them, living apart, is as a stranger to the fate of all the rest; his children and his private friends constitute to him the whole of mankind. As for the rest of his fellow citizens, he is close to them, but he does not see them; he touches them, but he does not feel them; he exists only in himself and for himself alone; and if his kindred still remain to him, he may be said at any rate to have lost his country.
Above this race of men stands an immense and tutelary power, which takes upon itself alone to secure their gratifications and to watch over their fate. That power is absolute, minute, regular, provident, and mild. It would be like the authority of a parent if, like that authority, its object was to prepare men for manhood; but it seeks, on the contrary, to keep them in perpetual childhood: it is well content that the people should rejoice, provided they think of nothing but rejoicing. For their happiness such a government willingly labors, but it chooses to be the sole agent and the only arbiter of that happiness; it provides for their security, foresees and supplies their necessities, facilitates their pleasures, manages their principal concerns, directs their industry, regulates the descent of property, and subdivides their inheritances: what remains, but to spare them all the care of thinking and all the trouble of living?
Thus it every day renders the exercise of the free agency of man less useful and less frequent; it circumscribes the will within a narrower range and gradually robs a man of all the uses of himself. The principle of equality has prepared men for these things; it has predisposed men to endure them and often to look on them as benefits.
Growing bureaucratization of our life (David Brooks)
It’s not only that growing bureaucracies cost a lot of money; they also enervate our society. They redistribute power from workers to rule makers, and in so doing sap initiative, discretion, creativity and drive.
High school students design their lives to fit the metrics that college admissions officers require. And what traits are selective schools looking for? They’re looking for students who are willing to conform to the formulas the gatekeepers devise.
People are weak, fragile, vulnerable and kind of stupid. They need administrators to run their lives. They have to be trained never to take initiative, lest they wander off into activities that are deemed by the authorities to be out of bounds.
The result is the soft despotism, a power that “is absolute, minute, regular, provident and mild.” This kind of power is now centerless. Presidents and executives don’t run companies, universities or nations. Power is now held by everyone who issues work surveys and annual reports, the people who create H.R. trainings and collect data.
Predictions (Nicholas Kristof)
None of us know what will happen, and it would be wise to be ready for anything.
天才(小野伸二)
(小野伸二は)プレー中に特別な映像が見えたことがあるのか? との質問に「ある」と回答。「プレー中というかトレーニングしている中で、常に敵や味方っていう映像(感覚)が全部あるわけですよ。普通のトレーニングしている時もそうだし、だからトラップの仕方とかも自分で変えていたし、ここに止めると敵がどう動くと想定しながらいつもやってたんで。みんなもそういうもんなんだと思ってた」と明かした。
続けて、それはプロでもふかんとして見えていたのか? と問われると、「みんなそうやって言うけど僕はそうじゃない。平面の映像で持っていたから。その前に自分で情報を集めていたので、だからすごい首は振ってました」と話した。
さらに「怪我以降、それが見えなくなったと?」と話を振られると、「そうです。それが一番驚きで、怪我から復帰してヤッターってワクワクして練習に行ったのに、何だろう今日は楽しいんだけど何か物足りない。アッ!! 映像が何もないぞと。ただ単にトレーニングしてるだけみたいな。あの映像はいつ戻ってくるのかと期待していたけれど、どれだけ時間が経っても戻らなかったですね」と衝撃のエピソードを披露。
番組ではどの時点での怪我だったのかは言及されなかったが、「だから、アレ以降いいプレーとういうか、アッと驚くようなプレーは出せなかったかもしれない。僕の中で最高のものは出せなかったかなと」と、自身の “サッカー人生” を大きく変えてしまった怪我を今でも残念がっている様子だった。
笹川良一、寺山修司
本当か嘘かは知らないが、笹川良一が競艇場に集まった競艇ファンを前にして、
「諸君がギャンブルに狂っているあいだに、諸君の妻や子は泣いている。こんなところに来てカネを賭けるようじゃいけない」
と説教を垂れたという。
また、これも本当か嘘かは知らないが、寺山修司が「天井桟敷」に劇を見に来る客について、
「劇を見て喜んでいるようではいけない。劇を見るのではなく、劇を演じるように生きなければ、何の意味もない」
と言ったらしい。
どちらの話も作り話だろうが、笹川良一と寺山修司の真髄をついてはいる。
競艇ファンがカネを賭けるおかげで天下国家を語ることができた笹川良一。
「天井桟敷」に来る客のおかげで好き勝手なことができた寺山修司。
どちらも普通ではない。
おもかさま(石牟礼道子)
「蓮の花はな」
ものやさしい声でおもかさまが言っている。めずらしいことに家族の会話にはいってきたのだ。
亀太郎がはっと座り直した。
「あい、蓮の花はな」
全員が耳を集中した。
「蓮の花は、あかつきの、最初の光にひらくとばえ。音立てて」
「音立てて、でござりやすか」
「菩薩さまのおらいますような音さてて、花びらが一枚ずつひらく」
「花びらが一枚ずつ」
「一枚ずつ、中に菩薩さまがおらいます」
白象に乗った菩薩さまの絵が床の間にあった。父が時おり、おもかさまは「常の人とはちがう」といって敬うことがこの時わかった気がした。
Tachyon
タキオン(tachyon)とは、常に光速よりも速く移動する仮想的な粒子である。ほとんどの物理学者は、光よりも速い粒子は既知の物理法則と一致しないため存在しないと考えている。仮にそのような粒子が存在し、光よりも速い信号を送ることができたとすると、相対性理論によれば因果律に反することになり、親殺しのパラドックスのようなタイプの論理的パラドックスが生じることになる。このような粒子が存在することを示す実験的証拠は見つかっていない。
タキオンは常に光よりも速く移動するので、それが近づいてくるのを見ることはできない。タキオンが近くを通過した後、観察者はそのタキオンの2つの像を見ることができ、それらは反対方向に現れて去っていく。この二重像効果は、超光速物体(この例では球体、透明な灰色で示されている)の通り道に直接位置する観測者にとって最も顕著なものである。タキオンは光よりも先に到着するため、球体が通過するまで観測者には何も見えず、その後(観測者の視点では)、到着する球体(右)と出発する球体(左)の2つに分かれて見える。
내일은 없다(윤동주) 明日はない(ユン・ドンジュ)
내일은 없다
ㅡ 어린 마음이 물은
내일 내일 하기에
물었더니
밤을 자고 동틀 때
내일이라고
새날을 찾던 나는
잠을 자고 돌아보니
그때는 내일이 아니라
오늘이더라
무리여! 동무여!
내일은 없나니
······
Keith Haring
大地震のテールリスク(菊池誠一)
南海トラフ巨大地震・首都圏大地震のような大地震が突然 起きた場合「どれだけの幅で株価が下がるのか}だが、日経平均株価でみて短期的には1万円を割ってしまうのは当然であり、場合によっては7000円割れ、最悪のシナリオを描くと5000円割れを覚悟すべきかもしれない。
次には「どれぐらいの間、株価低迷が続くのか」だが、場合によっては10年以上、あるいは20年間以上もかかって、やっと回復へといった状況も想定できる。内外の株式市場の歴史を振り返ると、株価低迷を生んだ原因はいろいろだが、20年間ぐらい低迷が続いたことは珍しくない。
為替相場については、常識的に考えれば、円相場が大きく下がるとみていい。海外から日本の株式、債券などに投入されている資金が、一斉に逃げ出そうとするからだ。しかし円相場が、たとえば対ドルでどこまで下がるのかとなると、事前にはなかなか読めない。一時的に1ドル=200円を超える水準にまで下がっても不思議ではない。
ただ、円相場について投資家が留意すべきことは、3・11が起きたとき、週が明けてからニューヨーク市場で円が急上昇し、歴史的な「円高現象」が出現したこと。その後も1年半にわたり円高が続き、日本株は低迷した。どうして円高になったのか。この点はいまだにわからない面が多い。研究者だけでなく、市場関係者の多くも疑問に思っているようだ。
南海トラフ巨大地震(経済的な被害)
南海トラフ巨大地震の被災地は中部地方、近畿地方、四国地方、九州地方を中心に超広域にわたり、地震動、液状化、津波による浸水及び火災等により、建物や資産、土地や交通施設等のインフラ・ライフライン等が著しく損壊する。
被災地には、我が国の経済を支えている地域が含まれ、鉄鋼業、石油化学工業、自動車製造業、船舶・航空機の製造業、電子・電気機器等の製造業が高度に集積していて、これらの産業を中心に全国・海外にまで相互に密接に関連するサプライチェーン・ネットワークが形成されている。このため、経済的な被害の影響は被災地内にとどまらず、全国・海外へと波及する。
被災地には、多くの農地や漁港、食料品工場等が集積している。このため、これらの被災により食料品や生活必需品の供給が滞ると、被災地外においても品不足とそれに伴う価格の高騰が生じ、市民生活に影響が及ぶ。
被災地は、東名・名神高速道路、東海道・山陽新幹線、名古屋港、大阪港、神戸港等が整備され、国内外における経済活動を支える人流・物流の大動脈となっている。これらの交通施設の損壊により物流が寸断されれば、燃料・素材・重要部品の調達が困難となるため、全国の生産活動が低下するとともに、港湾施設の被災により、輸出入の取り止めによる機会損失、代替輸送による時間損失やコスト負担が生じる。
生産活動の低下や物流寸断が長期化した場合、調達先を海外に切り替える動きが顕著となり、生産機能が国外流出する。工場等の喪失、生産活動の低下により、経営体力の弱い企業が倒産する。また、日本企業に対する信頼が低下し、株価や金利・為替の変動等に波及する。これらの影響が拡大すると、資金調達コストが増大し、企業の財務状況の悪化や倒産等が増加する。また、長期間にわたる生産活動の低下や海外貿易の滞りにより、海外に奪われた需要が地震発生前の水準まで回復せず、我が国の国際競争力の不可逆的な低下を招く。これらによる雇用環境の悪化や失業者の増加により、雇用者の所得が低下し、購買意欲を減退させるなど、景気停滞への負のスパイラルに陥る。経済活動の低下等による影響は、長期的な税収入の減少に結びつき、復旧・復興に要する財政出動と併せて、国や地方公共団体の財務状態が悪化する。また、日本経済に対する海外の信頼が低下し、海外からの資金調達コストが増大する。
産業の復興は、被災地における人員確保と生活再建が大前提となる。行方不明者の捜索活動や被災者の生活再建に時間がかかる場合、企業による早期の本格的な事業再開は見込めず、経済活動の低下が長期化し影響が拡大する。
沈黙・切支丹の里 (遠藤周作)
それには考えられる理由が当然ある。棄教者は基督教教会にとっては腐った林檎であり、語りたくない存在だからだ。臭いものには蓋をせねばならぬ。彼等の棄教の動機、その心理、その後の生き方はこうして教会にとって関心の外になり、それを受けた切支丹学者たちにとっても研究の対象とはならなくなったのである。
こうして弱者たちは政治家からも歴史家からも黙殺された。沈黙の灰のなかに埋められた。だが弱者たちもまた我々と同じ人間なのだ。彼等がそれまで自分の理想としていたものを、この世でもっとも善く、美しいと思っていたものを裏切った時、泪を流さなかったとどうして言えよう。後悔と恥とで身を震わせなかったとどうして言えよう。その悲しみや苦しみにたいして小説家である私は無関心ではいられなかった。彼等が転んだあとも、ひたすら歪んだ指をあわせ、言葉にならぬ祈りを唱えたとすれば、私の頬にも泪が流れるのである。
南海トラフ巨大地震
南海トラフ地震では静岡県から宮崎県にかけての一部で最大震度7になる可能性があると予想されており、九州から関東の太平洋では10mを超える大津波が想定されています。
その被害想定は下記の通りです。
・建物被害:2,386,000棟
・死者:323,000人
広域で震度7クラスの地震が予想されているのは、東海地震・南海地震・東南海地震の三つの地震が連動して発生する可能性があるためです。この三つの地震が同時に起こることを三連動地震と呼ぶこともあります。
また、東海地震・南海地震・東南海地震の震源域よりもさらに広域の震源域で地震が連動して発生する南海トラフ巨大地震が起きる可能性もあり、最大でM9.1が想定されています。その場合、高知県の土佐清水市や黒潮町では最大で34mの津波高が予想されており、これは10階建てビルに相当する高さです。
プライマリーバランス(Olivier Blanchard)
Divonne
West with the Night (Beryl Markham)
I have learned that if you must leave a place that you have lived in and loved and where all your yesteryears are buried deep, leave it any way except a slow way, leave it the fastest way you can. Never turn back and never believe that an hour you remember is a better hour because it is dead. Passed years seem safe ones, vanquished ones, while the future lives in a cloud, formidable from a distance.
Uncertainty
Life is inherently uncertain, and if you have difficulty dealing with that, you will have difficulty dealing with life.
Tolerating and even delighting in uncertainty doesn’t merely help us to accept life’s unpredictability; it also readies us to learn and adapt. Each day, the brain uses honed mental models about how the world works, which are used to process a shifting environment. When we meet something unexpected, a neural “prediction error” signals a mismatch between what we assumed would occur and what our senses tell us. Yet our uneasy sense of not knowing triggers a host of beneficial neural changes, including heightened attention, bolstered working memory and sensitivity to new information. The brain is preparing to update our knowledge of the world. Uncertainty offers the opportunity for life to go in different directions, and that is exciting.
This is why being open to uncertainty is critical for mental well-being.